It was good to be in on Monday, get a little bit of work done and it always seems to make the rest of the week feel a bit more manageable.
One of the highlights this week was heading up to watch Fulham vs Bournemouth with Kit. It was a fantastic game and such a good day out together. A massive thank you to Bob and Jenny, our lovely clients over at the Addlestone clinic, for sorting the tickets for us, we really appreciated it! Kit absolutely loved the whole experience and has been talking about it ever since.
Today, meanwhile, is officially Daddy Daycare. Charlotte’s up in London having a well-earned day with some of the nursery mums, a bit of pampering, relaxing, and adult conversation, which she thoroughly deserves. So I’m on full childcare duties today, which usually means a combination of footballs, snacks, refereeing sibling disputes and trying to keep everyone alive until bedtime.
We’ve also got our shutdown weeks coming up soon in the clinic, this is where the practitioners go away on holiday. I’m really looking forward to getting back into a full couple of weeks in clinic. I’ll be across both the West Byfleet and Addlestone clinics, so if you want to pop in, get checked over or just say hello, we’d love to see you.
Last week, we talked about sciatica one of the most common (and frustrating) types of pain I see in the clinic. If you’ve ever felt that sharp, shooting pain running from your lower back down your leg, you’ll know exactly what I mean.
But here’s where it gets a little more nuanced…
Not all “sciatica” is actually coming from your spine.
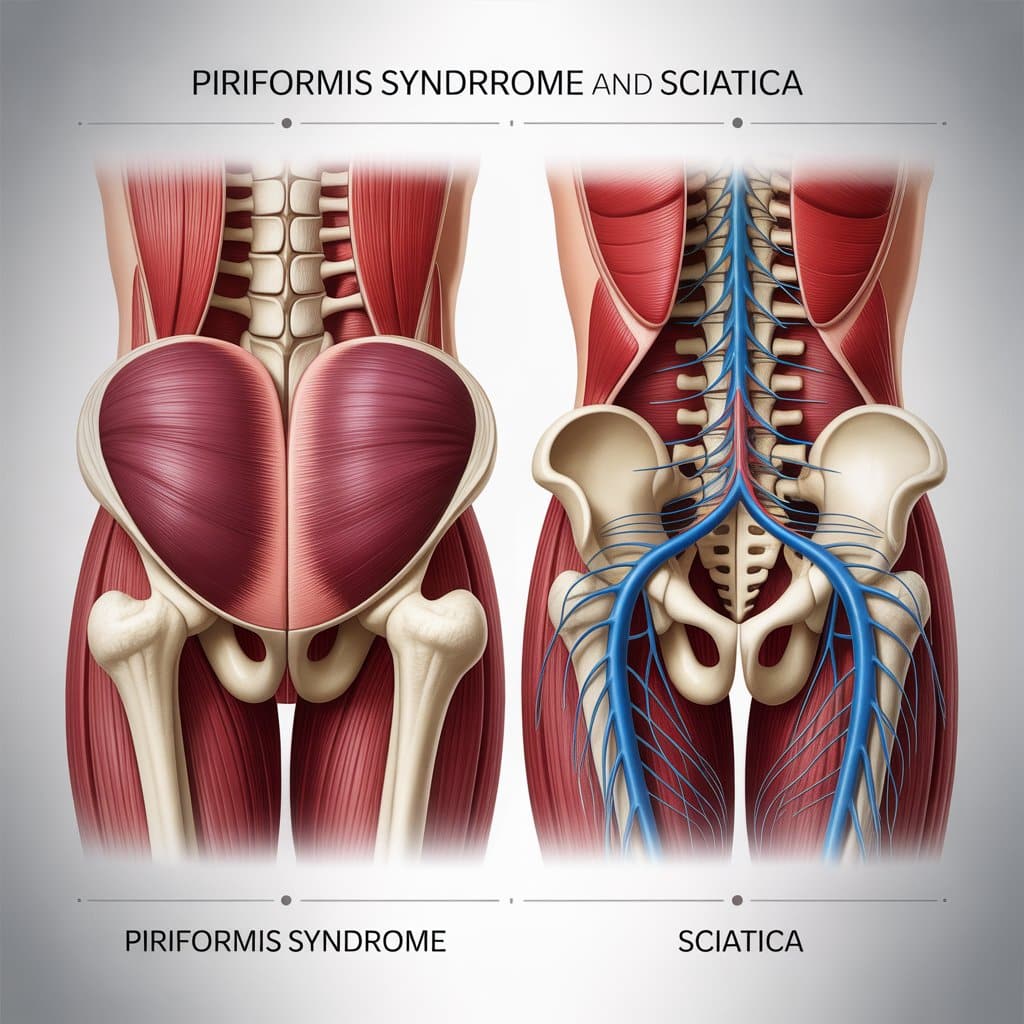
In fact, one of the most common conditions I see that mimics sciatica is something called piriformis syndrome. And while the symptoms can feel almost identical, the cause and therefore the treatment can be quite different.
Let’s break this down in a practical way so you can better understand what might be going on in your body.
What Is Sciatica?
Sciatica isn’t actually a condition itself, it’s a set of symptoms caused by irritation or compression of the sciatic nerve.
The sciatic nerve is the largest nerve in your body. It runs from your lower back, through your hips and glutes and all the way down each leg.
Common Symptoms of Sciatica:
- Sharp, shooting pain down one leg
- Tingling or “pins and needles”
- Numbness in the leg or foot
- Weakness in the leg
- Pain that worsens when sitting
In most cases, true sciatica originates from the lower spine, often due to:
- A bulging or herniated disc
- Spinal joint dysfunction
- Degenerative changes in the spine
I often explain it to patients like this: imagine a cable (your nerve) being irritated at its root in the spine. Everything downstream feels the effect.
What Is Piriformis Syndrome?
Let’s talk about the piriformis muscle.
This is a small, deep muscle located in your glutes, sitting very close to the sciatic nerve. Its job is to help rotate your hip.
In some people, the sciatic nerve actually runs through or very close to this muscle. So when the piriformis becomes tight, inflamed, or overworked, it can compress the nerve locally.
That’s what we call piriformis syndrome.
Common Symptoms of Piriformis Syndrome:
- Deep ache in the glute
- Pain that can radiate down the leg (similar to sciatica)
- Tenderness in the buttock
- Pain when sitting for long periods
- Discomfort when walking uphill or climbing stairs
So you can see why this gets confusing, the symptoms overlap a lot with sciatica.
Piriformis Syndrome vs Sciatica: Key Differences
Here’s where we start to separate the two.
1. Where the Problem Starts
- Sciatica: Originates in the lower back (spine)
- Piriformis Syndrome: Originates in the glute (muscle)
2. Type of Pain
- Sciatica: Often sharp, electric or burning
- Piriformis Syndrome: More of a deep, aching discomfort in the glute
3. Movement Patterns
- Sciatica: Bending, lifting or prolonged sitting may aggravate symptoms
- Piriformis Syndrome: Sitting and hip movements (like crossing legs) tend to worsen pain
4. Back Pain Presence
- Sciatica: Often includes lower back pain
- Piriformis Syndrome: Usually minimal or no back pain
Why This Difference Matters
This is really important.
Because if we treat piriformis syndrome like spinal sciatica or vice versa, we’re often missing the root cause.
I’ve seen patients spend months stretching their hamstrings or resting, thinking they’ve got “sciatica,” when actually the issue is a tight, overworked piriformis muscle.
And equally, I’ve seen people foam rolling their glutes endlessly when the real issue is a disc in the lower back.
The body is smart, but it can also be misleading.
What Causes Piriformis Syndrome?
In my experience, piriformis syndrome is often linked to lifestyle and movement patterns.
Common Triggers:
- Sitting for long periods (desk jobs, driving)
- Poor posture
- Weak glutes or core muscles
- Overtraining (especially running or cycling)
- Previous injuries
Think of it like this: if your bigger muscles aren’t doing their job properly, smaller muscles like the piriformis pick up the slack and eventually get overloaded.
What Causes Sciatica?
Sciatica tends to be more structural.
Common Causes:
- Disc bulges or herniations
- Spinal joint restrictions
- Poor spinal mechanics
- Repetitive strain or lifting injuries
As mentioned in our previous discussions, sometimes what feels like a “pulled muscle” is actually your body protecting something deeper, like a disc or nerve.
That protective response can create tightness, spasms and pain; But the root issue often lies beneath the surface.
How We Approach Treatment in the Clinic
This is where a proper assessment becomes key.
I always start by identifying:
- Where the pain is coming from
- How your body is moving
- What’s contributing to the problem
If It’s Sciatica (Spinal Origin):
We may focus on:
- Gentle spinal adjustments
- Spinal decompression therapy
- Improving joint mobility
- Reducing nerve irritation
If It’s Piriformis Syndrome:
We typically look at:
- Releasing tension in the piriformis muscle
- Improving hip mobility
- Strengthening surrounding muscles (glutes, core)
- Addressing posture and sitting habits
Sometimes, it’s actually a combination of both, which is more common than people think.
Simple Things You Can Start Doing Today
Regardless of which one you’re dealing with, there are some safe, general habits that can help:
1. Break Up Sitting Time
Try to stand up and move every 30–45 minutes.
2. Gentle Movement
Avoid complete rest. Light walking can often help reduce stiffness.
3. Posture Awareness
Keep your spine neutral when sitting, avoid slouching.
4. Stretching (With Caution)
- Glute stretches can help piriformis tightness
- But avoid aggressive stretching if pain is sharp or worsening
5. Listen to Your Body
Pain is information, not something to push through.
When Should You Seek Help?
If you’re experiencing:
- Persistent leg pain
- Numbness or tingling
- Pain that isn’t improving
- Difficulty sitting, walking or sleeping
…it’s worth getting it properly assessed.
The sooner we identify whether it’s piriformis syndrome, sciatica or a combination of both, the sooner we can guide you toward the right solution.
A Quick, Gentle Reminder
This blog is here to educate and guide, but it’s not a diagnosis.
Every body is different and the exact cause of your pain can vary based on your history, lifestyle and movement patterns.
Final Thoughts
Sciatica and piriformis syndrome can feel almost identical, but they’re not the same thing.
Understanding the difference is the first step toward getting the right care and more importantly, lasting relief.
If you’ve been dealing with ongoing leg or glute pain and you’re not quite sure what’s causing it, don’t guess your way through it.
We’re here to help.
If you’d like to understand what’s really going on and get a clear, personalised plan, feel free to book a discovery visit with us. We’ll take the time to listen, assess properly and guide you in the right direction.
References
- National Institute for Health and Care Excellence. (2020). Low back pain and sciatica in over 16s: Assessment and management (NICE Guideline NG59). NICE.
- Michel, F., Decavel, P., Toussirot, E., Tatu, L., Travers, V., Monnier, G., & Garbuio, P. (2013). Piriformis muscle syndrome: Diagnostic criteria and treatment of a monocentric series of 250 patients. Annals of Physical and Rehabilitation Medicine, 56(5), 371–383.
- Hopayian, K., Song, F., Riera, R., & Sambandan, S. (2010). The clinical features of the piriformis syndrome: A systematic review. European Spine Journal, 19(12), 2095–2109.
- Martin, H. D., & Reddy, M. (2011). The deep gluteal syndrome. Journal of Hip Preservation Surgery, 1(2), 99–107.
- Pinto, R. Z., Maher, C. G., Ferreira, M. L., Hancock, M., Oliveira, V. C., McLachlan, A. J., Koes, B., & Ferreira, P. H. (2012). Epidural corticosteroid injections in the management of sciatica: A systematic review and meta-analysis. Annals of Internal Medicine, 157(12), 865–877.